Previous issues
- Page Path
- HOME > Browse Articles > Previous issues
Original Articles
- The 2022 Annual Report on Toxicology Surveillance and Severe Poisoning Cases at Emergency Departments in Korea
- Eun Sun Lee, Su Jin Kim, Gyu Chong Cho, Mi Jin Lee, Byung Hak So, Kyung Su Kim, Juhyun Song, Sung Woo Lee
- J Korean Soc Clin Toxicol. 2023;21(1):1-16. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2023.00007
- 876 View
- 50 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Purpose: This study investigated the actual incidence of acute poisoning in Korea on a nationwide scale, with the aim of laying the groundwork for future initiatives in prevention, strategic antidote distribution, and the development of effective emergency treatment for acute poisoning.
Methods
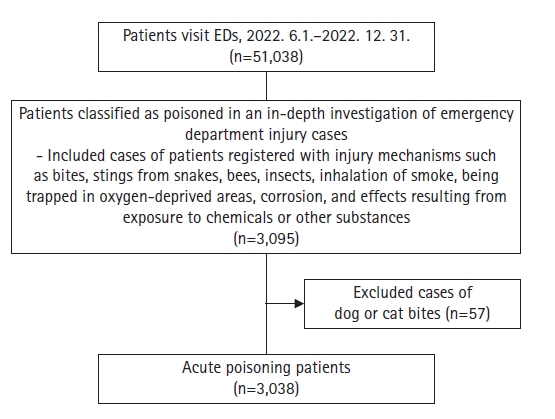
The study analyzed data from 3,038 patients who presented to emergency departments with poisoning-related conditions from June 1, 2022 to December 31, 2022 at 10 sites in nine cities across the country. We extracted data on general characteristics of the poisoning cases, including demographic characteristics (age and gender), place of exposure, reason for poisoning, route of exposure, and the substance involved in the poisoning incident. Age-related patterns in reasons for poisoning, medical outcomes, frequent and primary poisoning substances, and deaths were also analyzed.
Results
The population analyzed in our study was predominantly female, with women constituting 54.74% of all cases. Among infants and children, non-intentional poisoning due to general accidents was the most common cause, accounting for 71.43% of cases. Conversely, suicidal poisoning was more prevalent among teenagers and adults over 20. Fifty-two patients died during the study period, with males comprising approximately two-thirds (67.31%) of these fatalities. Pesticides were the most common poisoning substance among those who died, accounting for 55.77% of such cases. Notably, a significant majority of the victims were elderly individuals aged 60 and above.
Conclusion
This study holds substantial significance, since it represents the first comprehensive investigation and analysis of the symptoms, treatment, and causes of death due to poisoning in Korea on a national scale. By substantially expanding the range and types of poisonous substances examined, we were able to more precisely identify the characteristics and clinical patterns of poisoning cases nationwide.
- Association between continuous renal replacement therapy and mortality after acute herbicide (glyphosate and/or glufosinate) intoxication: propensity score matching approach
- Seung Woo Lee, Won-joon Jeong, Seung Ryu, Yongchul Cho, Yeonho You, Jung Soo Park, Changshin Kang, Hong Joon Ahn, So Young Jeon, Jinwoong Lee
- J Korean Soc Clin Toxicol. 2023;21(1):17-23. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2023.00001
- 423 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - Purpose: We investigated the association between continuous renal replacement therapy (CRRT) and mortality after acute glyphosate or glufosinate intoxication.
Methods
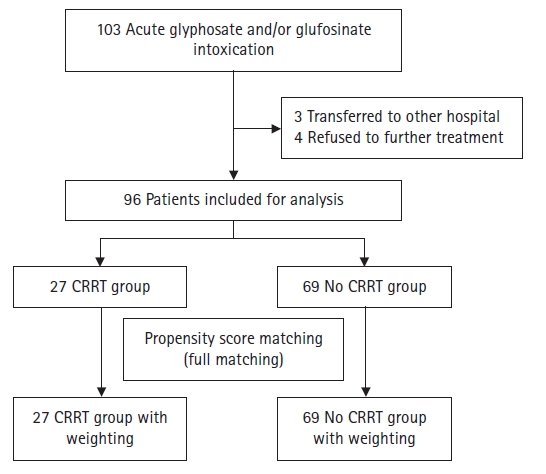
The electronic medical records of patients with acute herbicide ingestion who were admitted to the regional emergency center of a metropolitan city in Korea from 3/1/2013 to 2/28/2022 were analyzed and reviewed retrospectively. The case group received CRRT, while the control group did not. In total, 96 patients experienced acute herbicide intoxication in the study period. Baseline characteristics were analyzed and compared between the two groups after propensity score matching. The outcome variable was mortality fitted by a Cox proportional hazard model.
Results
After full matching between cases of CRRT use and controls (patients who did not receive CRRT) using propensity scores, 96 patients (27 cases, 69 controls) were analyzed. Propensity matching yielded adequate balance (standardized mean differences <0.25) for all covariates. We fit a Cox proportional hazards model with survival as the outcome and CRRT as a factor, including the matching weights in the estimation. The estimated hazard ratio was 0.41 (95% confidence interval, 0.23–0.76; p=0.0044), indicating that CRRT reduced mortality.
Conclusion
In this propensity score-matched analysis, CRRT reduced mortality in patients who visited the hospital with acute glyphosate or glufosinate intoxication. In patients with acute herbicide poisoning with high severity calculated by the APACHE II (Acute Physiology and Chronic Health Evaluation II) score and SOFA (Sequential Organ Failure Assessment) score, CRRT should be actively considered to improve the survival rate.
- Status and trends of medical expenditures for poisoning patients
- Eung Nam Kim, Soyoung Jeon, Hye Sun Lee, Sung Phil Chung
- J Korean Soc Clin Toxicol. 2023;21(1):24-31. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2022.00017
- 588 View
- 8 Download
-
 Abstract
Abstract
 PDF
PDF - Purpose: The purpose of this study was to estimate the medical expenditures for poisoning patients in Korea using data from National Health Insurance and the Korea Health Panel Survey.
Methods
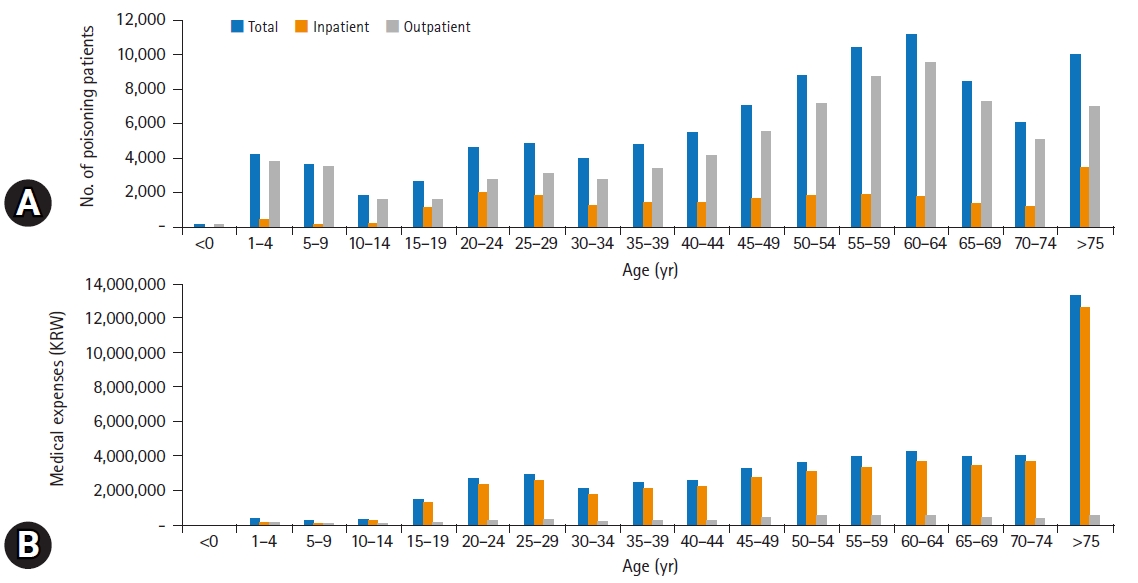
The operational definition of poisoning was the presence of Korean Standard Classification of Diseases codes from T36 to T65. The number of poisoning patients, the amount of legal copayments, and benefit and non-benefit costs were extracted from both databases. The frequency of emergency, inpatient, and outpatient treatment utilization by poisoning patients was determined, and medical expenses were calculated. Linear regression analyses were performed to investigate factors affecting the medical expenses of poisoning patients.
Results
The number of poisoning patients increased from 97,965 in 2011 to 147,984 persons in 2020. Medical expenses also increased by 74% from Korean won (KRW) 30.1 billion to KRW 52.3 billion, and benefit costs also increased by 79%. The average outpatient cost per person was KRW 67,660, and the inpatient cost was KRW 1,485,103. The average non-benefit medical expenses were KRW 80,298, accounting for about 16.2% of the total expenses. Multivariable analysis showed that the total expenditure was associated with economic status and disabilities.
Conclusion
The average medical expenditure per poisoning patient was KRW 534,302 in 2020, and poisoning-related costs gradually increased during the study period. Further research on the economic burden of poisoning should include indirect costs and reflect disease-adjusted life years.
- Changes in deoxyhemoglobin and admission duration in carbon monoxide poisoning patients: a retrospective study
- Jae Gu Ji, Yang Weon Kim, Chul Ho Park, Yoo Sang Yoon, Yundeok Jang, JI-Hun Kang, Chang Min Park, Sang Hyeon Park
- J Korean Soc Clin Toxicol. 2023;21(1):32-38. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2023.00004
- 734 View
- 14 Download
-
 Abstract
Abstract
 PDF
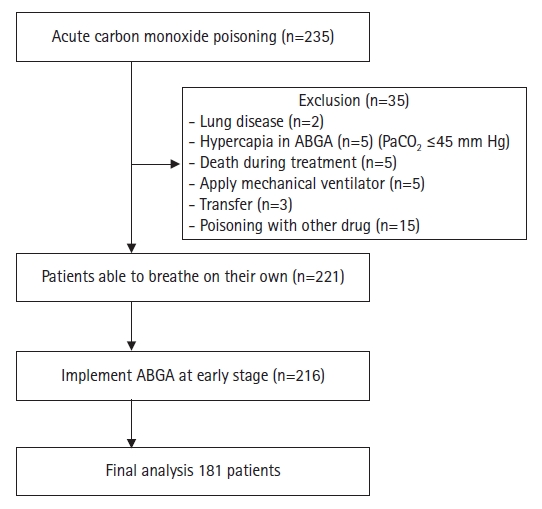
PDF - Purpose: The purpose of this study was to determine whether deoxyhemoglobin changes were associated with admission duration in carbon monoxide (CO)-poisoned patients.
Methods
This retrospective study included 181 patients who were able to breathe by themselves after CO poisoning. Arterial blood gas analysis was performed to measure their deoxyhemoglobin levels. Their baseline characteristics and clinical outcomes during hospitalization in the emergency department (ED) were collected and compared. To assess changes in deoxyhemoglobin levels, blood samples were taken immediately after patients presented to the ED and then again after 6 hours. For statistical analysis, logistic regression was utilized to determine the effect of deoxyhemoglobin changes on admission duration.
Results
The incidence rates of hypocapnia and hypoxemia at presentation after acute CO poisoning were 28.7% and 43.6%, respectively. Moreover, the magnitude of increasing deoxyhemoglobin levels in patients with hypoxemia (2.1 [1.7–3.1], p<0.001) and changes in deoxyhemoglobin levels appeared to have an impact on the length of hospitalization in the ED (odds ratio, 1.722; 95% confidence interval, 0.547–0.952; p<0.001).
Conclusion
In patients with acute CO poisoning, deoxyhemoglobin levels appeared to increase in those with hypoxemia, which in turn was associated with prolonged hospitalization.
- 2022 Annual Report of the Seoul Poison Control Center
- Yo Han Shin, Sijin Lee, Su Jin Kim, Young Hoon Yoon, Sung Woo Lee
- J Korean Soc Clin Toxicol. 2023;21(1):39-55. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2023.00006
- 1,037 View
- 20 Download
- 1 Citations
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
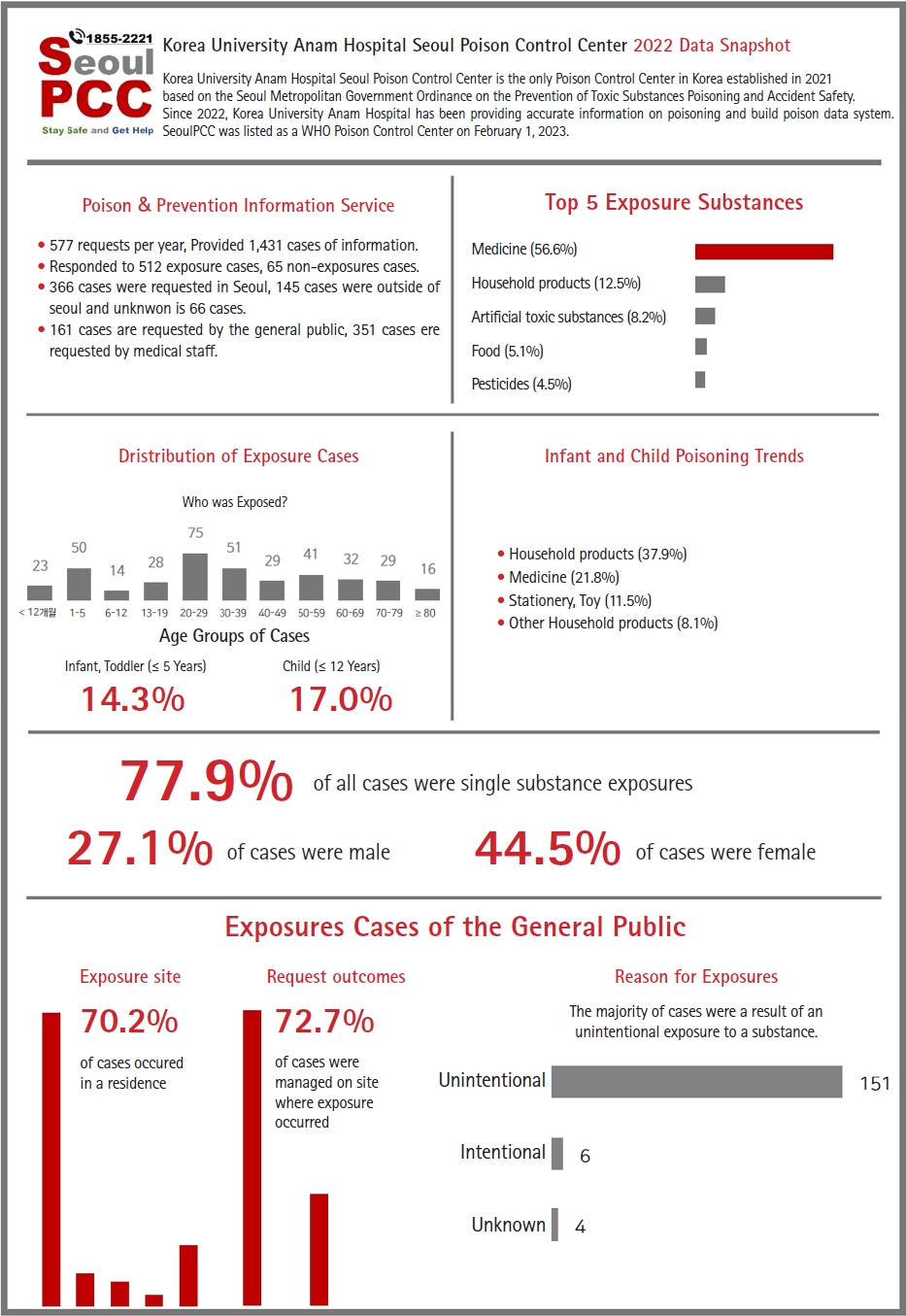
Supplementary Material - Purpose: The Korea University Anam Hospital Seoul Poison Control Center (SeoulPCC) was established in accordance with Seoul Metropolitan Government Ordinance No. 7524 “Seoul Metropolitan Government Ordinance on the Prevention of Toxic Substances Poisoning and Accident Safety.” Herein, the center’s annual performance in terms of project results and consultation information for 2022 are reported.
Methods
SeoulPCC operates a helpline (Help Call, 1855-2221) that the general public can use from 9:00 AM to 5:00 PM on weekdays, as well as chatting and chatbot counseling through KakaoTalk’s “Seoul Poison Control Center,” and one-on-one online counseling through the website. Additionally, it has constructed a system for communicating with the general public through social media. Poisoning disease information collected from SeoulPCC from January to December 2022 was analyzed according to the number of requests, age of exposure, gender, location, and reason. Requests from the general public were summarized, and a brief image presenting information on poisoning disease-related consultations was produced.
Results
SeoulPCC has a database containing information on 188,065 toxic substances collected by public institutions and provides this information to the general public and medical staff through its website. In 2022, consultations were performed through phone calls and SNS (social networking service) for 577 cases of poison information and first aid treatment due to exposure to toxic substances. There were 1,431 instances of providing poison information services. The annual requests included 512 exposure cases and 65 non-exposure cases. Furthermore, 366 cases were in Seoul, 145 cases were outside of Seoul, and 66 had an unknown location. The exposure cases included 161 requests from the general public and 351 requests from medical staff.
Conclusion
This is the first annual report in Korea to analyze the occurrence of poisoning based on consultations. It is of major significance that this report serves as a starting point for identifying and tracking the aspects and characteristics of poisoning cases in the pre-hospital stage. In the future, poisoning-related disease information provided through consultations and at the emergency room should be linked, and through real-time collection and analysis, this information should be used as basic data for poisoning disease management policies. -
Citations
Citations to this article as recorded by- Patterns of self-harm/suicide attempters who visited emergency department over the past 10 years and changes in poisoning as a major method (2011–2020)
Kyu Hyun Pai, Sung Woo Lee, Su Jin Kim, Kap Su Han, Juhyun Song, Sijin Lee, Ji Hwan Park, Jeijoon Song
Journal of The Korean Society of Clinical Toxicology.2023; 21(2): 69. CrossRef
- Patterns of self-harm/suicide attempters who visited emergency department over the past 10 years and changes in poisoning as a major method (2011–2020)
- Poisoning patients’ clinical features according to the blood level of propranolol
- Sungheon Kim, Byung Hak So, Hyung Min Kim, Kyeong Man Cha, Hwan Song, Won Jung Jeong
- J Korean Soc Clin Toxicol. 2023;21(1):56-63. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2023.00010
- 1,282 View
- 11 Download
-
 Abstract
Abstract
 PDF
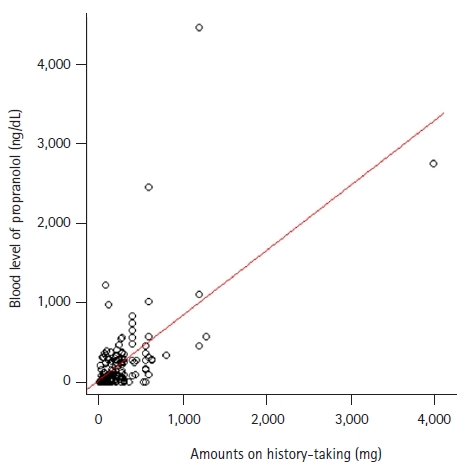
PDF - Purpose: Propranolol is widely prescribed to psychiatric patients to control adrenergic symptoms. However, propranolol poisoning can be fatal due to cardiovascular complications. We analyzed associations between blood levels of propranolol and patients’ clinical features, with the aim of predicting progression to severe complications.
Methods
Data were collected from patients aged 18 years or older who presented to the emergency department with propranolol poisoning between January 2016 and May 2022. We retrospectively analyzed their medical records and compared blood levels of propranolol between those who had cardiovascular complications and those who did not.
Results
Two hundred patients were included in this study. The blood levels of propranolol were significantly higher in patients with hypotension, bradycardia, and prolonged QT intervals, with median values of 247.0 ng/mL (interquartile range [IQR], 56.5–333.8 ng/mL), 275.8 ng/mL (IQR, 154.3–486.4 ng/mL), and 159.0 ng/mL (IQR, 33.9–310.8 ng/mL), respectively. In the predictive analysis of cardiovascular complications using a receiver operating characteristic curve, the area under the curve was 0.729 with a cut-off value of 72.40 ng/mL (sensitivity, 0.667; specificity, 0.819). In addition, the correlation coefficient between blood levels and the amount of drug described during the history-taking at the time of presentation was 0.634, which was found to have a significantly higher relationship.
Conclusion
Because blood levels of propranolol can be used as predictors of exacerbation in patients with propranolol poisoning, patients with blood levels above 72.40 ng/dL require careful treatment and observation from their initial presentation at the emergency department.
Case Report
- Pulmonary thromboembolism following organophosphate intoxication: a case report
- Ji Ho Lee
- J Korean Soc Clin Toxicol. 2023;21(1):64-67. Published online June 30, 2023
- DOI: https://doi.org/10.22537/jksct.2023.00002
- 380 View
- 16 Download
-
 Abstract
Abstract
 PDF
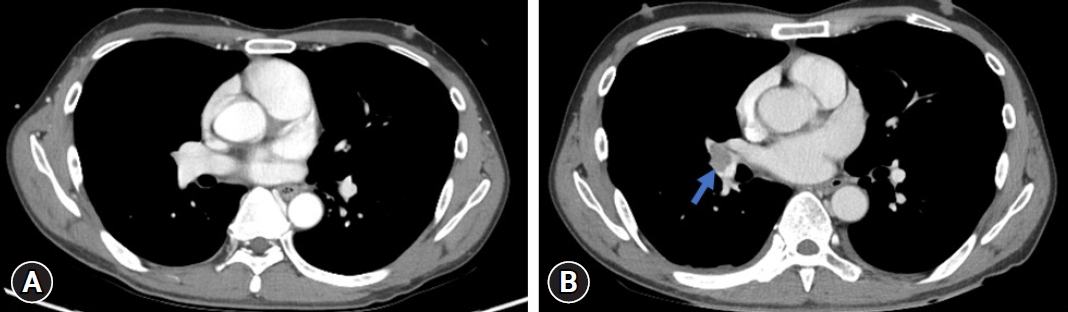
PDF - Various symptoms manifest after organophosphate intoxication due to muscarinic, nicotinic, and central nervous system effects. Complications are common, and morbidity occurs due to respiratory center depression, cardiovascular complications, aspiration pneumonia, general weakness, and neurological symptoms. Some studies have reported a statistically significant association between organophosphate intoxication and deep vein thrombosis. However, cases of pulmonary thromboembolism (PTE) resulting from organophosphate poisoning are very rare. A 45-year-old male patient was transferred to our hospital after ingesting an unknown amount of an insecticide and receiving 6 L of gastric lavage at a local hospital. Other than nausea, no symptoms (e.g., dyspnea) were present, but a hemodynamic test showed an elevated lactic acid level, and metabolic acidosis worsened over time. Accordingly, we conducted initial treatment including continuous renal replacement therapy. After 7 hours, the poisoning analysis result was confirmed, and lambda-cyhalothrin and chlorpyrifos (0.441 µg/mL and 0.401 µg/mL, respectively) were detected. We introduced pralidoxime. Although no increase in pseudocholinesterase was found during hospitalization, continuous renal replacement therapy and pralidoxime were discontinued because the patient did not show symptoms of intermediate syndrome, including dyspnea and altered consciousness. The patient complained of abdominal pain on hospital day 8. Abdominal computed tomography was performed to evaluate the possibility of a corrosive injury to the stomach or esophagus, and we confirmed PTE. The D-dimer level was 1.96 mg/L (normal range, 0–0.55 mg/dL). A radiologic examination showed a PTE in the main pulmonary artery leading to the segmental pulmonary artery. After heparinization, the patient was discharged after being prescribed a vitamin K-independent oral anticoagulant. Through this case, we would like to emphasize the need for a thorough evaluation of clinical symptoms because atypical symptoms can occur after poisoning with organophosphate pesticides.

 KSCT
KSCT



 First
First Prev
Prev



 Korean Society of Clinical Toxicology
Korean Society of Clinical Toxicology